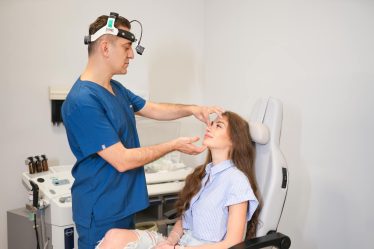
A rhinoplasty consultation should feel like a clinical assessment – not a sales appointment. This is where you confirm three things: (1) whether your goals are achievable for your anatomy, (2) whether function (breathing) is protected, and (3) whether the surgeon’s planning process is disciplined enough to deliver a stable long-term result.
Use the checklist below to steer the consult, compare surgeons fairly, and spot red flags early.
What to bring
Keep it simple, but arrive prepared:
- Your top 2-3 goals (e.g., reduce hump, refine tip, straighten, improve breathing)
- Any history of trauma, nasal surgery, chronic congestion, allergies, or snoring
- A list of medications/supplements and relevant medical conditions
- 3-5 reference photos showing the style you like (not “I want this exact nose”)
A good surgeon will use references to understand aesthetic direction (natural, refined, stronger bridge), while still explaining what’s realistic for your face.
High-value questions to ask (and what good answers include)
1) “Am I a candidate – and what limits my result?”
You want a surgeon who can clearly explain constraints like skin thickness, cartilage strength, asymmetry, previous trauma, or nasal valve support. The best answers include tradeoffs (for example, refinement versus structural stability). A “yes, easy” response with no nuance is not reassuring.
2) “What changes are you proposing, specifically?”
Push for plain-language specifics:
- Bridge: hump reduction, straightening, narrowing
- Tip: projection, rotation, refinement, symmetry
- Width: bones vs cartilage contributions
- Support: how the structure will be reinforced to prevent long-term collapse
If you leave without understanding the plan, you can’t properly consent.
3) “How will you evaluate breathing and function?”
Even if your goal is purely cosmetic, function matters. Ask how they assess:
- Septum deviation and turbinate issues
- Nasal valve support (a common cause of breathing problems)
- Whether functional steps may be needed alongside cosmetic changes
If function is brushed off or never mentioned, consider that a major gap in planning.
4) “Open or closed approach – what do you recommend and why?”
There isn’t one universally “best” approach. What matters is whether the surgeon can justify the approach based on your anatomy and goals. A good answer explains access/precision needs, scar placement, and how it may affect swelling and refinement.
5) “How do you plan for long-term stability?”
Rhinoplasty is not just shaping – it’s engineering. Ask how they prevent long-term issues like pinching, collapse, or shifting as swelling resolves and scar tissue forms.
Strong answers include discussion of structural support where needed (especially around the tip and valve area).
6) “What should I expect in 2 weeks, 6 weeks, 3 months, and 1 year?”
You want realism:
- Early swelling/bruising improves in the first weeks
- The nose can look “done” before it actually is
- Refinement continues for months; final definition often takes close to a year (sometimes longer)
If you’re promised “final results in a few weeks,” that’s a credibility problem.
7) “What complications do you see most often, and how do you handle them?”
Avoid surgeons who claim “no complications.” Instead, look for transparent discussion of:
- Bleeding/infection risk (and how it’s minimized)
- Prolonged swelling, asymmetry, scar tissue irregularities
- Breathing issues and how they’re assessed post-op
- What follow-up looks like if something isn’t healing as expected
8) “Who is performing the operation, and where?”
Confirm:
- The named surgeon is the primary operator
- Anaesthesia is handled by qualified staff
- The facility has appropriate standards and emergency protocols
Clarity here is basic due diligence.
9) “Can I see before-and-after cases similar to me?”
Ask to see consistent photos (same lighting/angles), multiple views (front/profile/base), and cases that match your starting anatomy (skin thickness, nasal shape, prior trauma). Be skeptical of heavily filtered images or inconsistent photography.
Red flags that should make you pause
These patterns tend to correlate with poor expectation management or weak process:
- Guaranteed outcomes or “perfect” promises
- “We can make you look exactly like this celebrity/photo”
- Minimal exam (no functional discussion, no structural assessment)
- A scripted consult that feels rushed or sales-led
- One-size-fits-all language (“just shave the bump and refine the tip”)
- Dismissive communication when you ask about risks, timelines, or limitations
- Unclear post-op pathway (who you contact, how often you’re reviewed, how issues are handled)
Rhinoplasty is a long recovery with normal ups and downs; you want a clinic that can support you through that process calmly and competently.
How to decide after the consult
After you leave, do a quick reality check:
- Do I understand the plan and its limitations?
- Did they address function and breathing appropriately?
- Did I feel pressured – or informed?
- Was the follow-up pathway clear and structured?
If any of these are “no,” a second opinion is reasonable. In rhinoplasty, careful planning and communication are not “nice to have” – they are core safety features.
If you’re researching rhinoplasty in London, prioritize surgeons who explain tradeoffs clearly, assess function seriously, and show consistent outcomes in comparable cases.
Ready for your rhinoplasty in London?
A strong rhinoplasty consultation should give you a tailored surgical plan, clear expectations for recovery, and transparency about risk and follow-up. Ask specific questions, watch for red flags, and choose the surgeon whose process feels methodical – not persuasive.